Disulfiram, a well-established medication for the treatment of alcoholism, has helped people addicted to cocaine reduce abuse of the drug from 2.5 days a week to 0.5 days a week on average. The finding builds on previous studies in which NIDA-funded researchers demonstrated the medication's promise in two subgroups of cocaine abusers—alcoholics and those with co-occurring opioid addiction. Their current results suggest that disulfiram is effective in treating the general population of cocaine-addicted patients, including those who are nonalcoholic. The medication's effectiveness in nonalcoholic patients adds to evidence that disulfiram works directly to reduce cocaine abuse rather than indirectly by reducing concurrent alcohol abuse. The investigators also found that, like disulfiram, cognitive-behavioral therapy (CBT) reduced cocaine abuse by 2 days.
Dr. Kathleen Carroll and her colleagues at Yale University School of Medicine in New Haven, Connecticut, treated 121 outpatients for 12 weeks. The 32 women and 89 men met the criteria for cocaine dependence specified in the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV) and reported abusing cocaine 13 days on average during the month and 2.5 days during the week before treatment. During the study, each patient received either 250 mg/day of disulfiram or placebo and participated in weekly individual sessions of behavioral therapy, either CBT or IPT (interpersonal psychotherapy). CBT coaches patients to recognize and cope with situations that tend to induce drug craving and abuse. In IPT, patients clarify and address key personal problems related to the substance abuse. On average, patients attended eight behavioral therapy sessions. The type of therapy did not affect rates of treatment completion.
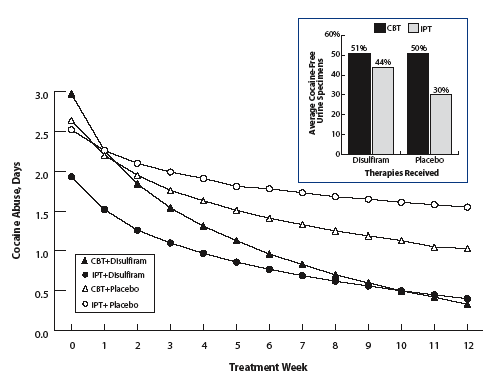 Both Disulfiram and CBT Help Patients Reduce Cocaine Abuse. Over the 12-week study, patients taking disulfiram or participating in cognitive-behavioral therapy (CBT) demonstrated greater reductions in cocaine abuse than those taking placebo or receiving interpersonal psychotherapy (IPT).
Both Disulfiram and CBT Help Patients Reduce Cocaine Abuse. Over the 12-week study, patients taking disulfiram or participating in cognitive-behavioral therapy (CBT) demonstrated greater reductions in cocaine abuse than those taking placebo or receiving interpersonal psychotherapy (IPT).All patients abused cocaine on fewer days during treatment than they had in the weeks before. The extent of recovery depended on the therapy. By the end of treatment, patients taking disulfiram reduced weekly cocaine abuse by 2 days on average, compared with 1 day for those taking the placebo, no matter which psychotherapy group they participated in. Similarly, patients who participated in CBT reduced weekly cocaine abuse by 2 days on average, compared with 1 day for IPT participants regardless of which medication they received. The data were based on self-reported cocaine abuse, but weekly urine tests generally corroborated (84 percent) patient information. More urine samples from participants receiving disulfiram and CBT (51 percent), placebo and CBT (50 percent), and disulfiram and IPT (44 percent) were cocaine negative during the study than those from participants taking the placebo and IPT combination (30 percent); the latter demonstrated the least favorable treatment outcomes.
Dr. Carroll and her colleagues verified compliance with the daily medication regimen by testing urine samples for tracers that were added to the medication and the placebo. Taking the capsules every day was associated with better outcomes among patients who received either disulfiram or placebo, although disulfiram's effectiveness remained superior to placebo's when the researchers took medication compliance into account. Dr. Carroll emphasizes that "not taking medication can undercut the benefits of all pharmacotherapies, and an important goal of behavioral therapy is improvement of medication compliance." Dr. Dorynne Czechowicz of NIDA's Division of Clinical Neuroscience, Development and Behavioral Treatment says the findings highlight the importance of integrating addiction medication and behavioral treatment. "All patients in the study participated in some form of behavioral therapy, which facilitated recovery from substance abuse and helped patients stick to the medication regimen," she says.
Disulfiram had a more pronounced benefit for patients who were not alcohol-dependent at the outset of the study and for those who abstained from alcohol during the study. Patients who drank while taking disulfiram tended to take less of the medication than those who did not drink. Instead of deterring drinking and thereby reducing cocaine abuse, the unpleasant physical consequences of mixing alcohol with the medication led patients to stop taking disulfiram when they wanted to drink or abuse cocaine. "These findings seem to validate the clinical observation that patients have to stop drinking before they can kick cocaine abuse," says Dr. Carroll. Patients participating in CBT showed better outcomes than those in IPT, regardless of concurrent drinking. CBT, a well-established behavioral treatment, might be the best option for some patients, including those facing co-occurring alcohol and cocaine addiction, she says. Patients without concurrent alcoholism may be candidates for disulfiram, CBT, or a combination.
Disulfiram interacts with cocaine to produce an unpleasant sense of hyperstimulation. In laboratory studies, people experiencing a disulfiram-cocaine interaction demonstrated increased heart rate and blood pressure and reported anxiety, paranoia, and restlessness. Animal studies suggest that disulfiram, like cocaine, enhances the activity of the neurotransmitter dopamine. Possibly, when someone has taken disulfiram, subsequent administration of cocaine elevates dopamine to excessive levels that produce discomfort and aversion. Animal research suggests that disulfiram increases levels of dopamine by blocking an enzyme that breaks dopamine down. People with low levels of the enzyme, dopamine-β-hydroxylase (DBH), have increased dopamine activity. Hormones, as well as genes, may influence DBH levels. Researchers suspect that estrogen hormones increase DBH, attenuating the effect of disulfiram, which could explain why women seem to benefit less than men.
Source
- Carroll, K.M., et al. Efficacy of disulfiram and cognitive behavior therapy in cocaine-dependent outpatients: A randomized placebo controlled trial. Archives of General Psychiatry 61(3):264-272, 2004. [Abstract]
Disulfiram May Work for Men, but Not Women
Researchers studying disulfiram, an "old" medication for alcoholism that has emerged as a potential "new" treatment for cocaine abuse, have found a possible sex difference in treatment response: Cocaine-addicted men who were treated with the medication had better outcomes than those who were not, whereas women showed no significant difference in outcome.
Dr. Kathleen Carroll of Yale University School of Medicine and her colleagues have conducted several studies on the medication's effects on cocaine abuse and have moved on to the next step—determining which types of patients benefit from the treatment. There were not enough women in their recent study to analyze sex differences, so the investigators combined data from two of their other treatment studies to compare men's and women's responses to disulfiram. "We know that men and women react to cocaine differently. For example, women progress more quickly to cocaine addiction than men. Sex differences in treatment response seemed likely," says Ms. Charla Nich, lead investigator of the study.
In one study, the investigators treated alcohol- and cocaine-addicted patients with disulfiram and various behavioral therapies; in the second, they tested disulfiram in opioid- and cocaine-addicted patients under treatment with methadone. Altogether, 191 patients participated in the studies, which, when combined, had enough women (36 percent) to permit a valid comparison.
Both studies found that patient groups taking disulfiram reduced cocaine abuse compared with groups receiving placebo. But when the investigators combined and reanalyzed the data, they found that only the men in the groups responded to the medication. The reanalysis indicated that men treated with disulfiram produced a higher percentage of drug-free urine specimens than men in the placebo groups (49 versus 30 percent). Among women, however, the percentage of drug-free specimens was not significantly different with disulfiram or placebo (38 versus 39 percent).
"Our data don't conclusively prove a sex difference in the response to disulfiram," says Ms. Nich. "For that, we need studies that directly compare men and women taking the medication." NIDA's Dr. Dorynne Czechowicz agrees that researchers should follow up on these intriguing preliminary findings, which "highlight the importance of paying attention to sex differences in medication development and other drug abuse research."
Source
- Nich, C., et al. Sex differences in cocaine-dependent individuals' response to disulfiram treatment. Addictive Behaviors 29(6):1123-1128, 2004. [Abstract]
