Chronic cocaine abusers may feel they are sleeping better and better during early abstinence, but objective measures show the opposite happens. A team of NIDA-funded addiction and sleep researchers at the Yale and Harvard Schools of Medicine found evidence of insomnia, with learning and attentional deficits, on days of taking the drug and after 2.5 weeks of abstinence. The researchers believe cocaine may impair the brain's ability to gauge its own need for sleep, and patients' ability to benefit from early treatment may suffer as a result.
"Problems in memory and attention are linked with increased treatment dropout and likely affect patients' ability to 'take in' lessons from drug abuse counseling," says Dr. Robert Malison of Yale, a co-investigator on the study. If the results are confirmed, clinicians and patients may want to consider addressing sleep disorders in early therapy, perhaps with the use of medications or behavioral treatments.
The researchers recruited 10 men and two women aged 24 to 49 who, on average, had abused cocaine for 17 years and had used $500 worth of the drug per week. All the participants declined an offer of drug abuse treatment. Urine tests indicated that cocaine was the only drug any of them had abused during the week before the study.
At the outset of the study, participants self-administered cocaine from a pump under physician oversight, building up to a dose of 32 mg/kg of body weight over 1.5 hours, then repeating this dose essentially at will, but no less than 5 minutes apart, for another 1.5 hours. Subsequently, they self-administered the higher dose with the same minimal restriction for 2 hours on each of three consecutive days, either on days 4-6 or 18-20. This schedule simulated chronic cocaine abusers' typical bingeing pattern of drug abuse and allowed researchers to monitor each participant's sleep and cognitive performance for 17 days after a binge.
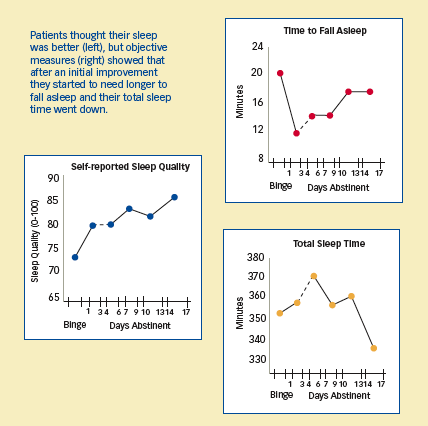 Objective Measures Belie Patient's Impressions of Sleep Improvement: Patients thought their sleep was better (left), but objective measures (right) showed that after an initial improvement they started to need longer to fall asleep and their total sleep time went down.
Objective Measures Belie Patient's Impressions of Sleep Improvement: Patients thought their sleep was better (left), but objective measures (right) showed that after an initial improvement they started to need longer to fall asleep and their total sleep time went down.Research staff made sure the participants stayed awake from 7:45 AM to 9:30 PM, and let them sleep through the night. At night, the participants wore Nightcap sleep monitors, a bandana-like device that records eye and body movements that indicate whether someone is awake, asleep and dreaming, or sleeping dreamlessly. On most nights participants also wore polysomnographic (PSG) devices that continuously assessed brain activity with electroencephalography (EEG) and measured eye and muscle movements associated with different sleep stages. Combining the information gathered by these measures with participants' responses to daily questionnaires on their sleep experience and with cognitive testing, the researchers demonstrated that the participants had:
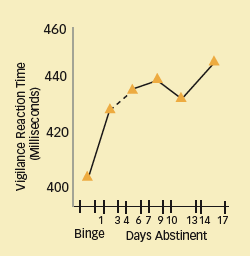 Alertness Impairments Parallel Sleep Deficits: In the Digital Vigilance Test, participants were required to press a button when they saw a target number on the right side of the screen while viewing a rapidly changing number sequence in the middle of the screen. Poor performance on the task corresponded with sleep deficits at 14-17 days of abstinence.
Alertness Impairments Parallel Sleep Deficits: In the Digital Vigilance Test, participants were required to press a button when they saw a target number on the right side of the screen while viewing a rapidly changing number sequence in the middle of the screen. Poor performance on the task corresponded with sleep deficits at 14-17 days of abstinence.- Sleep deficits—After 14 to 17 days of abstinence, the study group exhibited sleep deficits on several measures, relative to healthy, age-matched peers who participated in prior studies. For example, they had less total sleep time (336 versus 421-464 minutes) and took longer to fall asleep (19 versus 6-16 minutes).
- Declines in sleep quantity and quality—The time participants took to fall asleep and their total time asleep transiently improved during the first week of abstinence, but then reverted to the patterns recorded on days of cocaine taking. On abstinence days 14-17, participants took an average of 20 minutes to fall asleep (from a low of 11) and slept for 40 minutes less than their minimum. Slow-wave sleep—a deep sleep that often increases following sleep deprivation—rose during the binge and on abstinence days 10-17.
- Lack of awareness of their sleep problems—In contrast to the evidence of objective measures, the study participants reported steadily improving sleep from the beginning to the end of their days of abstinence.
- Impairments in learning and attention—As with sleep quality, participants' performance on tests of alertness and motor-skills learning initially improved and then deteriorated. On abstinence day 17, they registered their lowest scores on alertness and ability to learn a new motor skill.
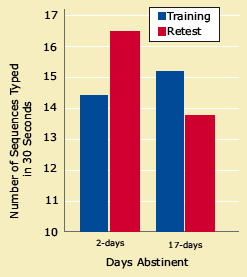 Performance Declines With Sleep Quality: In the Motor-Sequence Task, participants typed a five-digit sequence of four keys with their non-dominant hand, a skill that improves after a night's sleep. Cocaine abusers showed improvement after two but not 17 days of abstinence.
Performance Declines With Sleep Quality: In the Motor-Sequence Task, participants typed a five-digit sequence of four keys with their non-dominant hand, a skill that improves after a night's sleep. Cocaine abusers showed improvement after two but not 17 days of abstinence.Increased Risk of Relapse
"Unlike most people with chronic insomnia, including alcoholics, cocaine abusers do not perceive sleep problems and may not ask clinicians for treatment to improve sleep," says Dr. Malison. The problem often goes unaddressed and persists as a result, and the accompanying impairments in attention and learning may affect how well they respond to drug abuse treatment (see "Cocaine Abusers' Cognitive Deficits Compromise Treatment Outcomes"). Clinical studies have shown that poor objective sleep during the first 2 weeks of abstinence predicts relapse to alcohol 5 months after treatment.
In fact, the insidious nature of cocaine-related insomnia may directly trigger relapse, suggests Dr. Peter Morgan, lead investigator of the study. "Addicted people may take cocaine to improve sleep-related cognitive functioning deficits—unaware that they are abusing, in part, to 'solve' these problems."
Dr. Morgan adds, "Cocaine abusers who recognize their cognitive problems often report that it takes them 6 months to a year to turn the corner—a clinical observation that points to the need for longer term studies of sleep and treatment outcomes among this population." In addition to studies with larger numbers of participants, the investigators say there is a need to investigate possible gender differences in cocaine-related sleep problems. Dr. Morgan and his team are currently testing two medications, tiagabine and modafinil, to see if they can improve cocaine abusers' sleep and restore cognitive performance.
"Experts believe that not getting enough sleep is an unmet public health problem in the general population. These findings highlight this important problem in cocaine abusers," says Dr. Harold Gordon of NIDA's Division of Clinical Neuroscience and Behavioral Research.
Source
Morgan, P.T., et al. Sleep, sleep-dependent procedural learning and vigilance in chronic cocaine users: Evidence for occult insomnia. Drug and Alcohol Dependence 82(3):238-249, 2006. [Abstract]
