Findings from a recent NIDA-funded study represent early fruits of research on a recently recognized network of brain circuits. Dr. Elliott Hong and colleagues at the University of Maryland School of Medicine and collaborators at the NIDA Intramural Research Program showed that the strength of one of these "resting-state" circuits correlates with individuals' vulnerability to nicotine dependence. Moreover, this circuit appears to mediate the increases in dependence associated with an important genetic risk factor.
 Head Shot: In this diffusion spectrum image, fiber bundles are color coded according to their directions of impulse transmission. The Human Connectome Project uses diffusion spectrum and other cutting-edge neuroimaging techniques to map fiber pathways in the normal human brain. (For more images, see http://www.humanconnectomeproject.org/gallery/
Head Shot: In this diffusion spectrum image, fiber bundles are color coded according to their directions of impulse transmission. The Human Connectome Project uses diffusion spectrum and other cutting-edge neuroimaging techniques to map fiber pathways in the normal human brain. (For more images, see http://www.humanconnectomeproject.org/gallery/Dr. Marcus E. Raichle and colleagues at the Washington University School of Medicine in St. Louis opened the door to the study of resting-state circuits about 10 years ago when they noted that some brain regions synchronize their activity when individuals are awake and alert but are not performing any specific task. The researchers suggested that these inter-regional interactions provide an intrinsic functional organization of the brain. In addition to Dr. Hong's recent research, other studies have borne out this idea, for example by identifying what appear to be resting-state neural signatures for different types of mental illness.
The initial observations of resting-state circuits were made with functional magnetic resonance imaging (fMRI) data obtained while individuals were idle between cognitive tasks. Such data are routinely produced in fMRI studies but had generally been regarded as simply byproducts of studies that focused on the brain's activity during task performance. Today, however, many research teams are conducting studies specifically to generate resting-state data. NIDA and other agencies within the National Institutes of Health are supporting this work for the light it may shed on questions related to their respective missions. Research on resting-state circuits promises to yield insights into how the brain works at a hitherto unexplored basic level.
Circuit Responses to Nicotine
Dr. Hong and colleagues set out to identify resting-state circuits related to nicotine dependence and to assess the impact of nicotine replacement therapy on those circuits. They focused on circuits that include the cingulate cortex because activity in that brain region appears to be disrupted in addiction (see "Methamphetamine Abusers Show Increased Distractibility").
The researchers recruited 19 healthy smokers, ages 18 to 50, who were not trying to quit. Each participant underwent fMRI brain imaging in two sessions spaced roughly a week apart. The brain images were obtained while participants rested after performing cognitive tasks for an hour. The participants wore a nicotine patch during one of the imaging sessions and a placebo patch during the other.
The results revealed that the cingulate forms resting-state circuits with 56 of the many brain areas to which it connects anatomically. Several of these circuits were sensitive to nicotine: Their strength—the degree of synchronization between their component areas—markedly increased when participants wore the nicotine patch.
Most of the nicotine-sensitive circuits connect the cingulate with cortical areas that influence thinking, attention, and memory. A few of the nicotine-boosted pathways connect the cingulate with the postcentral gyrus, a cortical region that processes sensory information.
"The enhanced communication of cingulate-frontal cortex circuits after nicotine administration may underlie the well-documented transient cognitive boost from nicotine," says Dr. Hong.
A Circuit for Severity
The Maryland team found that the severity of nicotine addiction was associated with a circuit that connects the dorsal portion of the anterior cingulate cortex (dACC) to the ventral striatum. Participants with weaker communication in this circuit scored higher on the Fagerström Test for Nicotine Dependence (see graph below).
The dACC supports impulse and emotional control, which are impaired in addiction. The striatum processes rewards including the pleasure derived from smoking. "Communication strength within the circuit, rather than the activity of the individual areas, seems to relate to the severity of nicotine dependence among smokers," Dr. Hong says.
Unlike the cingulate-cortex circuits, communication in the dACC-striatum circuit was similar whether the participants wore the nicotine patch or placebo patch. Dr. Hong and colleagues suggest that this observation may shed light on a clinical conundrum: If people smoke primarily to obtain the effects of nicotine and avoid withdrawal, why is it that some 85 percent of people who try the patch keep on smoking?
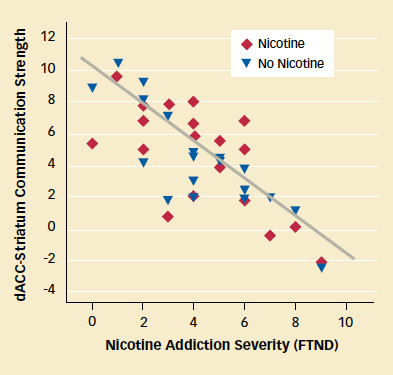 Nicotine Addiction Linked With Weak Communication in Circuit: Smokers with greater dependence on nicotine, as evidenced by higher scores on the Fagerström Test for Nicotine Dependence (FTND), demonstrated weaker communication in a brain circuit connecting the dorsal anterior cingulate cortex (dACC) and the striatum. Communication strength was similar with and without a nicotine patch, suggesting that this circuit is unresponsive to the medication.
Nicotine Addiction Linked With Weak Communication in Circuit: Smokers with greater dependence on nicotine, as evidenced by higher scores on the Fagerström Test for Nicotine Dependence (FTND), demonstrated weaker communication in a brain circuit connecting the dorsal anterior cingulate cortex (dACC) and the striatum. Communication strength was similar with and without a nicotine patch, suggesting that this circuit is unresponsive to the medication."Our finding that the circuit linked with severity of dependence was unresponsive to a nicotine replacement dose is quite provocative," says Dr. Hong. "It may be one reason why nicotine replacement therapies do not have overwhelming success at helping people quit."
A Pathway for Risk
In a second study, the Maryland team produced evidence that a gene variant that increases the risk for smoking dependence does so, in part, by weakening the dACC-striatum resting-state circuit. The researchers also implicated the circuit in the increased susceptibility to smoking addiction seen among individuals with certain mental illnesses.
The 184 adult participants who underwent fMRI in this study included smokers, nonsmokers, and ex-smokers. The researchers determined each participant's genotype for the α5 subunit of the nicotinic acetylcholine receptor (nAChR). The α5 subunit is abundant in the cingulate, ventral striatum, and extended amygdala areas, and one of its variants—designated rs16969968—increases the risk for smoking dependence.
The α5 risk variant was associated with decreased strength in the dACC-striatum circuit among both smokers and nonsmokers. Among smokers, the circuit influenced vulnerability to smoking dependence more strongly than the gene variant. "Decreased strength in the dACC-striatum brain circuit explained approximately 10 to 12 percent of the differences in nicotine dependence among smokers," Dr. Hong says. "In contrast, genotype alone accounted for only 1 to 4 percent." These results suggest that the α5 risk variant interacts with other genes or environmental factors to weaken the circuit and increase vulnerability.
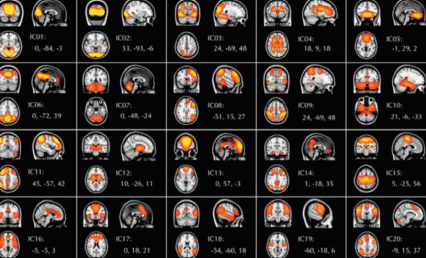 Seeing the Connections: 20 Resting-State Circuits Revealed: Resting-state functional magnetic resonance imaging (R-fMRI) shows brain circuits that can be identified when people are alert but not doing any particular task. Analyses of scans from more than 1,000 healthy adults revealed 20 resting-state brain networks. Each one is shown here in coronal, sagittal, and transverse views. The colors in these composite images show the statistical robustness of these patterns in each brain region, with yellow indicating the greatest statistical significance; orange, an intermediate level; and red, the least. From the supplement to Proceedings of the National Academy of Sciences 107(10): 4734-4739, 2010.
Seeing the Connections: 20 Resting-State Circuits Revealed: Resting-state functional magnetic resonance imaging (R-fMRI) shows brain circuits that can be identified when people are alert but not doing any particular task. Analyses of scans from more than 1,000 healthy adults revealed 20 resting-state brain networks. Each one is shown here in coronal, sagittal, and transverse views. The colors in these composite images show the statistical robustness of these patterns in each brain region, with yellow indicating the greatest statistical significance; orange, an intermediate level; and red, the least. From the supplement to Proceedings of the National Academy of Sciences 107(10): 4734-4739, 2010.Among the participants in this study were 76 individuals with mental disorders including schizophrenia, substance dependence, and anxiety and depressive disorders. This group had weaker dACC-striatum circuit strength and higher smoking rates than participants without mental disorders. They were not more likely to have the high-risk α5 gene variant, however, suggesting that other genes or other factors underlie the relative weakness in their circuitry. One possibility is that as-yet-unidentified gene variants may simultaneously predispose certain individuals to mental illness and disrupt the circuit.
"These findings are important because they change the way scientists think about nicotine's influence on the brain and provoke many new hypotheses for future imaging research," says Dr. Steven Grant of NIDA's Division of Clinical Neuroscience and Behavioral Research. For example, he says, researchers might test whether behavioral therapy or other smoking cessation treatments strengthen the connection and whether the strength of the circuit increases over time with abstinence.
Mapping the Brain's Functional Circuits
In addition to investigating the involvement of specific brain pathways in disorders, scientists are striving to achieve an overall understanding of brain circuitry and its functioning. Two projects exemplify different approaches to accumulating and organizing the extensive data needed to develop brain maps and test hypotheses. One, the 1000 Functional Connectomes Project (FCP), applies a community-wide data-sharing effort among neuroscientists that took its inspiration from the 1000 Genomes Project that helped map the human genome. The other, the Human Connectome Project (HCP), is a prospective in-depth investigation of 1,200 individuals that will also be widely shared with the scientific community.
"The 1000 FCP takes a discovery-science approach, capturing many neural networks that researchers examine in specialized studies. The HCP drills down to provide the rigorous details of brain circuitry," says Dr. Grant. "Brain science will benefit from both types of projects."
The 1000 Functional Connectomes Project
In the 1000 FCP, scientists from around the world deposited previously collected resting-state brain scan data into an open-access database (http:// fcon_1000.projects.nitrc.org). In what is, at times, a competitive research environment, these investigators agreed to make their data freely available because they recognized the value that a large-scale repository offers to the neuroscience community. The project has accumulated resting-state brain scan data from more than 1,400 study participants scanned at 35 neuroimaging centers.
Any investigator can download data from the ever-expanding collection and use it to search for resting-state pathways or test hypotheses about how the brain works. To date, researchers have downloaded data from the project's Web site more than 38,000 times.
In an initial paper announcing the 1000 FCP, contributing researchers described 20 functional networks that were identified by analyzing brain scans of 1,093 individuals at 24 imaging centers. The group included NIDA-funded researcher and 1000 FCP project advisor Dr. F. Xavier Castellanos of New York University (NYU) and project co-founders Drs. Michael P. Milham of NYU and Bharat B. Biswal of New Jersey Medical School.
"The full number of functional networks remains to be seen—estimates range up to several hundred, depending upon the criteria and approaches used to define them," says Dr. Milham. The 20 circuits identified by the team (see graphic above) were consistently present in both males and females regardless of age, but some varied in strength depending on gender and age. Other researchers have also noted variations in the strength of certain circuits, which may be clues to differences in behaviors.
Brain Mapping Across the Decades
Since the mid-to-late 1970s, neuroscientists have used structural magnetic resonance imaging (MRI) and other techniques to map the brain's anatomical structures. But anatomy does not provide a complete picture of how the brain works.
The early 1990s saw the advent of functional MRI (fMRI), which maps changes in brain activity rather than anatomy. In a typical fMRI experiment, scientists scan the brain while a study participant experiences particular stimuli or performs assigned mental tasks. Such studies have identified brain circuits that underlie specific behaviors and has provided pieces of the functional map, also known as the functional connectome.
Before 2001, most scientists doing fMRI experiments ignored so-called deactivations—the tendency for some brain regions to become less active when participants switch from rest to performing a task. However, Dr. Marcus E. Raichle and colleagues at the Washington University School of Medicine in St. Louis noted that a pattern of consistent deactivations could be identified during almost any task and that the brain consumes a great deal of energy whether or not individuals are performing specific tasks. Using a technique called resting-state functional MRI, Dr. Raichle and other neuroscientists discovered that when the brain is at rest, its activity patterns are not random. Analysis of its synchronized activity patterns has begun to reveal the brain's overall functional organization.
Source
Raichle, M.E. A paradigm shift in functional brain imaging. Journal of Neuroscience 29(41):12729-12734, 2009. (Full Text (PDF, 721KB))
"The team's observation of distinct functional networks indicates that there is a fundamental organizational principle to the brain that all humans share," says Dr. Grant.
Dr. Castellanos says that neuroscientists participating in the 1000 FCP also plan to build brain scan repositories for two critical populations—youths and people with psychiatric disorders. Drs. Milham and Castellanos and their colleagues at the Nathan Kline Institute for Psychiatric Research have also provided an open dataset of 207 individuals. It includes a range of brain imaging measures and an extensive set of behavioral information—including psychiatric interviews, exercise fitness, metabolic measures, and the amount of food eaten in a controlled meal. These data, from individuals aged 6 to 85, most of whom are free of psychiatric diagnoses, are available to scientists at http://fcon_1000.projects.nitrc.org/indi/pro/nki.html.
"The 1000 FCP has achieved a huge normative brain imaging dataset at a relatively low cost because scientists volunteered to share data and work together," says Dr. James Bjork of NIDA's Division of Clinical Neuroscience and Behavioral Research. "If this spirit of collaboration takes hold in sub-areas of neuroimaging—among the many research groups studying depression, for example—many discoveries will be possible."
The Human Connectome Project
The National Institutes of Health Blueprint for Neuroscience Research is sponsoring the HCP, which will map the neural circuitry of the normal adult brain using a battery of cutting-edge and traditional techniques. According to the HCP Web site, the project's goal is an unparalleled compilation of neural data and an interface to "navigate the brain in a way that was never before possible; fly through major brain pathways, compare essential circuits, zoom into a region to explore the cells that comprise it and the functions that depend on it."
Starting in 2012, HCP scientists will perform high-resolution resting-state fMRI and diffusion imaging on 1,200 healthy adults. To make possible studies of the heritability of brain circuits and their associated traits, the study population will include 300 twin pairs and their siblings. Some study participants will also undergo traditional fMRI, which documents brain changes during the performance of tasks, and magneto/electroencephalography. The images obtained will be made freely available to researchers, along with the study participants' genotypes and results on tests of sensory, motor, and cognitive function. A supercomputer and a user-friendly toolbox of advanced computer programs will be available for researchers who wish to use the resulting vast datasets to answer questions about brain structure and function.
The foundational work for the HCP is being conducted by consortiums between the University of California, Los Angeles, and Massachusetts General Hospital, and between Washington University, St. Louis, and the University of Minnesota, Twin Cities. Information on the current status and future plans can be found at http://www.humanconnectomeproject.org/ and http://humanconnectome.org.
Future Clinical Tools
"The brain maps that ultimately will arise from repositories that combine imaging and behavioral information will be very useful to clinicians," says Dr. Castellanos. As a pediatric psychiatrist, he anticipates someday using maps of typical brain development, just as clinicians use physical growth charts, to assess children's progress and catch problems early.
Dr. Castellanos predicts that psychiatrists may eventually use brain scans in diagnosing mental disorders, just as cardiologists use electrocardiograms in diagnosing heart disease. "Current psychiatric diagnosis is based on symptoms, but different causes and underlying circuits can produce the same or similar symptoms. Brain maps can greatly advance the identification of particular mechanisms underlying neuropsychiatric disorders," Dr. Castellanos says. Brain maps could also provide a basis for tracking the effects of interventions, thereby speeding the development of evidence-based preventive measures and treatments targeting drug addiction and other mental illnesses.
Sources
Biswal, B.B., et al. Toward discovery science of human brain function.Proceedings of the National Academy of Sciences 107(10):4734-4739, 2010. (Full Text (PDF, 754KB))
Hong, L.E., et al. A genetically modulated, intrinsic cingulate circuit supports human nicotine addiction. Proceedings of the National Academy of Sciences107(30):13509-13514, 2010. (Full Text (PDF, 819KB))
Hong, L.E., et al. Nicotine addiction and nicotine's actions are associated with separate cingulate cortex functional circuits. Archives of General Psychiatry66(4):431-441, 2009. (Full Text (PDF, 1.3MB))
