A new analysis of data from a trial in which intensive case management (ICM) outperformed usual care among women receiving welfare (see “Intervention Improves Abstinence, Employment Among Welfare Recipients”) indicates that comorbid depression played a significant role in the outcomes. Dr. Alexis Kuerbis and colleagues at Columbia University found that both assignment to ICM and the presence of high levels of depression symptoms independently enhanced participants’ likelihood of engaging in substance abuse treatment and attending more treatment sessions during the 2-year study. Surprisingly, ICM proved to be more effective among depressed participants than among nondepressed ones in improving two outcomes: treatment engagement and reducing alcohol consumption. A higher level of depression symptoms at the start of the study also predicted more days of abstinence over a 2-year period.
The researchers had hypothesized that ICM would be less, rather than more, effective for depressed women, as it did not include any specialized focus on comorbid psychiatric disorders. To explain their contrary findings, the researchers note previous research that showed that depression increases readiness to change. They suggest that ICM participants’ copious ongoing contact with case managers and help in overcoming practical barriers to treatment capitalizes on such readiness.
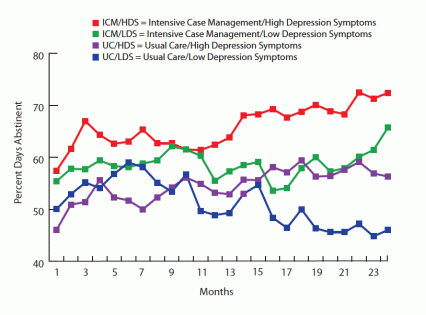 Higher Depression Levels Associated With More Days of Abstinence Among substance-abusing women receiving welfare benefits, a higher level of depression symptoms at the start of the study predicted more days of abstinence over a 2-year period.
Higher Depression Levels Associated With More Days of Abstinence Among substance-abusing women receiving welfare benefits, a higher level of depression symptoms at the start of the study predicted more days of abstinence over a 2-year period.The study was conducted in Essex County, New Jersey, with 302 women who were receiving Temporary Assistance for Needy Families. The new analysis included data from 294 participants who filled out the Beck Depression Inventory-II at the beginning of the study. Fifty-two percent scored 20 or above on the index, which is the conventional threshold for a diagnosis of major depression. These women were roughly evenly distributed between the two treatment groups.
Journal of Studies on Alcohol and Drugs 72(2):297–307, 2011. Abstract Available
