A study strongly suggests that offering jail detainees effective evidence-based treatment for substance use disorders can reduce the Nation’s burden of HIV. Researchers found that, among a large cohort of HIV-infected jail detainees, those who had used illicit drugs in the month before becoming incarcerated reported lower levels of engagement in HIV treatment than those who had not recently used illicit drugs.
From 2007 to 2011, Dr. Ehsan Chitsaz at Yale University School of Medicine, Dr. Frederick Altice at the Yale School of Public Health, and colleagues recruited the largest cohort of HIV-infected jail detainees assembled to date for any study: 1,166 adults from 10 study sites in 9 states. The NIDA-supported team assessed the participants’ involvement in the HIV continuum of care and also obtained demographic and social data, including details about their drug use. Overall, 72 percent of the detainees reported using drugs in the 30 days before incarceration; almost two-thirds had Addiction Severity Index (ASI) scores that met the DSM-IV criteria for a substance use disorder.
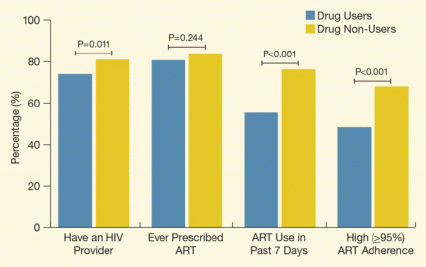 Figure. HIV-Infected Jail Detainees Who Have Used Drugs in the 30 Days Before Incarceration Are Less Engaged in the HIV Continuum of Care Compared with HIV-infected detainees without a recent history of drug abuse, those who used drugs within the 30 days before incarceration showed significantly lower levels of accessing an HIV care provider, having a prescription of ART in the last 7 days, and optimal adherence levels to their ART regimen.
Figure. HIV-Infected Jail Detainees Who Have Used Drugs in the 30 Days Before Incarceration Are Less Engaged in the HIV Continuum of Care Compared with HIV-infected detainees without a recent history of drug abuse, those who used drugs within the 30 days before incarceration showed significantly lower levels of accessing an HIV care provider, having a prescription of ART in the last 7 days, and optimal adherence levels to their ART regimen.
- Text description of Figure
-
The figure shows a bar graph indicating the proportion (as percentage) of HIV-infected jail detainees who are actively engaged in HIV treatment. The vertical (y)-axis shows the percentage engaged in treatment, and the horizontal (x)-axis shows the type of HIV treatment or type of indicator for involvement in HIV treatment (i.e., having an HIV care provider, having ever been prescribed antiretroviral therapy [ART], having used ART in the past 7 days, and having high [95 percent or more] adherence to ART). Among jail detainees who used drugs in the 30 days before their incarceration (blue bars), consistently fewer were engaged in any of the four HIV-treatment indicators than among those who did not use drugs during that same time period (yellow bars). Drug use decreased the proportion of those having an HIV care provider by 7 percentage points, having ever been prescribed ART by 3 percentage points, having used ART in the past 7 days by 21 percentage points, and having high adherence to ART by 20 percentage points. The differences were statistically significant for having an HIV care provider (p=.011), as well as for having a prescription of ART in the last 7 days and for optimal adherence levels to their ART regimen (p<.001), but not for having ever been prescribed ART (p=0.244).
Individuals reporting drug abuse in the 30 days before they had entered jail were less likely to:
- Have a regular HIV care provider.
- Have used antiretroviral therapy (ART) in the 7 days before incarceration.
- Have high enough levels of HIV medication compliance (adherence of 95 percent or more to a treatment regimen) to achieve viral suppression (see Figure).
The research team also reported that a 10 percent increase in the severity of a subject’s addiction to illicit drugs reduced the likelihood that he or she had an HIV care provider by 12 percent, of receiving ART by 19 percent, and of closely adhering to HIV-medication regimens by 16 percent. In contrast, the severity of alcohol use did not significantly correlate with these worsening outcomes.
Approximately 1 in 6 of the 1.2 million HIV-infected people in the United States pass through the criminal justice system every year. Despite the high proportion of jail detainees who use drugs, most receive only limited evidence-based treatment for their drug problems. The Yale researchers reason that with increased effective substance abuse treatment leading to enhanced HIV treatment engagement and outcomes in this population, overall HIV transmission rates could drop significantly—particularly as drug users with HIV are at relatively high risk of transmitting the virus to others.
In additional studies with the same HIV-infected cohort, Dr. Altice and colleagues have shown that HIV-infected women detainees especially stand to benefit from effective substance abuse treatment during their incarceration. These studies also suggest that making effective substance abuse treatment available to detainees in jail, along with continuing care post-release, can reduce homelessness and recidivism during detainees’ transition from jail back into their communities.
This study was supported by NIH grant DA017072 and by the Health Resources and Services Administration.
Source:
Chitsaz, E.; Meyer, J.P.; Krishnan, A.; Springer, S.A.; Marcus, R.; Zaller, N.; Jordan, A.O.; Lincoln, T.; Flanigan, T.P.; Porterfield, J.; Altice, F.L. Contribution of substance use disorders on HIV treatment outcomes and antiretroviral medication adherence among HIV-infected persons entering jail. AIDS Behavior. 17(Suppl. 2): S118-127, 2013. Full Text
