Intensified screening for HIV among injection drug users receiving opioid agonist therapy could prevent more than twice as many new infections as current screening practice, NIDA-supported researchers estimate. The findings from the recent study suggest that screening every 6 months instead of annually, and adding viral RNA testing to the currently used HIV antibody testing, could improve both effectiveness and cost-effectiveness (see Figure 1). The benefits would accrue from flagging new infections and initiating treatment sooner.
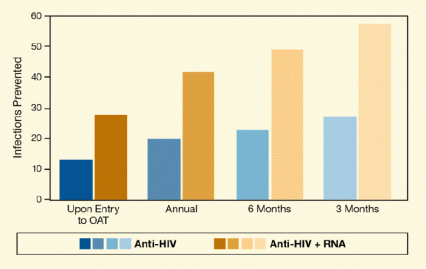 Figure 1. More Frequent and Expanded Screening for HIV Infection Is Predicted To Prevent New HIV Infections in Users of Injection Drugs Testing for HIV antibodies and RNA yielded a greater reduction of new infections than testing for HIV antibodies alone. Increasing the frequency of tests, starting at entry to opioid agonist therapy (OAT), also decreased the number of new infections.
Figure 1. More Frequent and Expanded Screening for HIV Infection Is Predicted To Prevent New HIV Infections in Users of Injection Drugs Testing for HIV antibodies and RNA yielded a greater reduction of new infections than testing for HIV antibodies alone. Increasing the frequency of tests, starting at entry to opioid agonist therapy (OAT), also decreased the number of new infections.
- Text description of Figure 1
-
The figure shows a bar graph indicating the number of HIV infections averted with different screening strategies. The vertical (y)-axis shows the number of infections averted, and the horizontal (x)-axis shows the screening strategy (i.e., screening upon entry of opioid agonist therapy [OAT], annually, semiannually, or quarter-annually). Screening was for HIV antibodies only (Anti-HIV; blue bars) or for both HIV antibodies and HIV RNA (Anti-HIV + RNA; beige bars). Screening on entering ORT averted the fewest HIV infections (less than 15 and less than 30 for Anti-HIV and Anti-HIV + RNA screenings, respectively) and each step toward more frequent screening (i.e., annual, semiannual, or quarter-annual screening) increased the number of HIV infections averted. At each screening frequency, screening for both HIV antibodies and RNA consistently yielded a higher number of infections averted than screening for HIV antibodies only. The highest number of prevented HIV infections (almost 60) was achieved with screening for HIV antibodies and RNA every 3 months, whereas screening only for HIV antibody at the same frequency averted only about 25 HIV infections.
Dr. Lauren E. Cipriano and colleagues at Stanford University in California used mathematical modeling to assess the impacts of several HIV screening strategies on new HIV infections in a virtual city with 2.5 million people aged 15 to 59 years. The researchers used published demographic and health data to give the virtual city a profile that is representative of large U.S. cities, including a 1.2 percent prevalence of injection drug use, and a 6.5 percent prevalence of HIV among the injection drug users. They used published data on screening results, HIV transmission, HIV progression, and the effects of treatment to estimate the number of infections that each strategy could prevent over a 20-year period.
Of all the screening strategies the researchers put into the mix, semiannual testing for HIV antibodies and HIV RNA yielded the best combination of effectiveness and cost-effectiveness. A critical advantage of this strategy is that HIV RNA testing reliably detects HIV disease in the acute stage, when it is largely invisible to antibody testing. During this stage, which lasts up to 3 months following acquisition of the virus, HIV is highly active and transmissible. Accordingly, informing patients of their infection, counseling them on ways to avoid transmitting the virus, and starting antiretroviral therapy to suppress viral activity can significantly impede the spread of the disease.
Dr. Cipriano and colleagues’ model predicts that each diagnosis of acute HIV in an injection drug user undergoing opioid agonist therapy would avert 1.3 new HIV infections over 20 years, provided antiretroviral therapy was initiated immediately after the diagnosis. Altogether, the intensified screening strategy would prevent 49 HIV infections over the 2 decades, compared to 20 that would be prevented by the current practice of screening annually for antibodies alone. Although injection drug users would be the only ones screened, approximately half of the averted infections would have occurred in nonusers of injected drugs.
The Stanford team calculated that, compared to annual HIV antibody screening, the intensified screening would gain an additional 286 quality-adjusted life years (QALYs) over 20 years. The QALY is a measure of the health impact of a condition or intervention that takes into account its effect on function and happiness in everyday life as well as longevity. With 1 QALY representing 1 full year lived in complete mental and physical health, the researchers posited that the average healthy nonuser of injection drugs in their virtual city would experience 0.9 QALY per year, and the average injection drug user would experience 0.75 QALY per year.
For their cost-effectiveness estimates, the researchers considered outlays for screening and treatment of detected cases. They concluded that, compared to annual HIV antibody screening, the intensified screening strategy would cost an additional $46,000 for each QALY gained (see Figure 2). Health economists often consider interventions that cost up to $100,000 per QALY to be cost-effective.
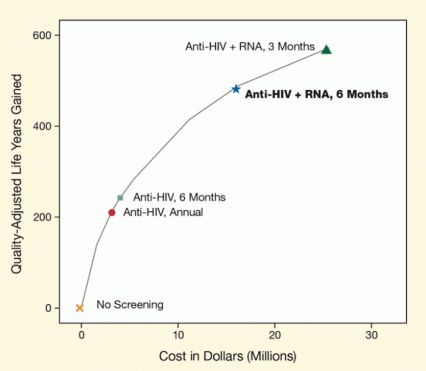 Figure 2. Screening for Anti-HIV Antibodies and RNA Every 6 Months Is Projected To Be More Effective Than Annual Screening for Anti-HIV Antibodies Only Testing for both HIV antibodies and RNA every 6 months (in bold and marked with blue star) was projected to gain 492 quality-adjusted life years (QALYs) at a cost of $65,900 per QALY. In comparison, annual testing for HIV antibodies alone gained 206 QALYs at a cost of $20,075 per QALY gained. The $46,000 difference in cost per QALY with the intensified screening is within a range generally considered to be cost-effective for interventions.
Figure 2. Screening for Anti-HIV Antibodies and RNA Every 6 Months Is Projected To Be More Effective Than Annual Screening for Anti-HIV Antibodies Only Testing for both HIV antibodies and RNA every 6 months (in bold and marked with blue star) was projected to gain 492 quality-adjusted life years (QALYs) at a cost of $65,900 per QALY. In comparison, annual testing for HIV antibodies alone gained 206 QALYs at a cost of $20,075 per QALY gained. The $46,000 difference in cost per QALY with the intensified screening is within a range generally considered to be cost-effective for interventions.
- Text description of Figure 2
-
The figure shows a plot depicting quality-adjusted life years (QALYs) gained as a result of HIV screening and the costs of four different HIV screening strategies. The vertical (y)-axis shows QALYs gained, and the horizontal (x)-axis shows the cost (in U.S. dollars) of each screening strategy. Costs represent the total expenditures for screening and HIV treatment in a population of 2,100 injection drug users in ORT at any one time. Screening annually for HIV antibodies only (anti-HIV, annual; red circle) cost $2.87 million and resulted in 206 QALYs gained, semiannually for HIV antibodies only (anti-HIV, 6 months; small square) cost $3.80 million and resulted in 237 QALYs gained, semiannually for HIV antibodies and RNA (anti-HIV + RNA, 6 months; blue star) cost $16.20 million and resulted in 492 QALYs gained, and quarter-annually for antibodies and RNA (anti-HIV + RNA, 3 months; blue star) cost $25.67 million and resulted in 574 QALYs gained.
Early Diagnosis and Treatment
“The lack of frequent and expanded testing for HIV in users of injection drugs is a missed public health opportunity,” says Dr. Cipriano. “If at least 50 percent of individuals identified with acute HIV can be referred to treatment, then adding viral RNA detection to antibody screening protocols is cost effective.”
Another takeaway from the study, says Dr. Cipriano, is that counseling injection drug users in risk reduction can reduce the human and financial costs of HIV. “Durable changes in behavior are difficult to achieve, but if such changes are realized, they can have a large impact on reducing transmission of HIV and hepatitis C. Connecting effective risk-reduction counseling with HIV screening may even reduce the risk-taking behaviors of uninfected users of drugs,” she says.
Dr. Cipriano stresses that the virtual city her team created for their mathematical modeling is only broadly representative of a typical large U.S. city, and localities need to adapt their screening to their specific situations. For example, in their study, the researchers found that the cost-effectiveness of the semiannual screening strategy depended on the prevalence of HIV that they attributed to the injection drug users in their virtual city. Other factors such as the availability of programs to treat drug dependence, and of other harm-reduction services such as needle exchange, can also affect the cost-effectiveness of screening.
Dr. Peter Hartsock of NIDA’s Epidemiology Research Branch highlights that the findings of the study support the idea that intensified screening can help catch HIV infection at its onset. “Early diagnosis of HIV is critical because of the high viral load found at this acute stage, increasing the risk of transmission,” he says.
Recent results from epidemiological and mathematical modeling studies have contributed to the current focus on implementing programs for HIV detection, treatment, and prevention using the model “Seek-Test-Treat-Retain.” Dr. Hartsock comments that acceptance of this approach has been helped by the fact that HIV carries less stigma today than in the past: The routine implementation of HIV testing programs has led to a normalization in the perception of this disease, and better options for treating HIV infection have lowered the level of anxiety associated with its diagnosis.
This study was supported by NIH grant DA15612.
Source
Cipriano, L.E., et al. Cost effectiveness of screening strategies for early identification of HIV and HCV infection in injection drug users. PLoS ONE 7(9):e45176, 2012. Full Text
