A new pharmacological approach being developed by NIDA-supported scientists has the potential to make treatment for human immunodeficiency virus (HIV) disease easier and more effective. Called nano-antiretroviral therapy (nano-ART), the approach turns macrophages—one of the very cell types that HIV uses to replicate and spread through the body—into carriers for anti-HIV medications.
A recent study with animals furthers hopes that nano-ART can relieve the current need for copious, tightly scheduled pill regimens that can challenge patients’ ability to adhere to a treatment. The study also indicated that nano-ART might more effectively attack HIV in viral reservoirs into which current medications do not penetrate. These reservoirs, which exist even when patients take all of their pills diligently, stand in the way of a cure for HIV and may incubate resistant viral strains.
Riding With the Cavalry
Nano-ART is an example of an approach called cell-mediated medication delivery, which researchers are exploring for a variety of clinical applications. The approach aims to manufacture nano-formulations made of particles with optimum excipients, shape, size, and charge to facilitate the uptake of HIV medications into immunocytes (cells of the immune system). Immunocytes make near-ideal carriers for medications because they circulate to nearly all of the tissues in the body and rally to sites of infection or injury. In principle, they thus can deliver medications precisely to where they are most needed.
Moreover, once inside immunocytes, nano-formulated medications are sheltered from degradation by enzymes that break down conventional medications, including antiretrovirals. The nano-formulations enter intracellular compartments called endosomes, which gradually discharge them back out into the surrounding blood or tissues over time. As a result, they may yield high and stable concentrations of medication for extended periods of time.
For nano-ART, Dr. Yazen Alnouti and colleagues at the University of Nebraska Medical Center in Omaha created nano-formulations of the antiretroviral medications, atazanavir (ATV) and ritonavir (RTV). The researchers packaged crystals of ATV and RTV into nanoparticles coated with a synthetic polymer called poloxamer 188, which has properties that promote uptake into macrophages.
In the study, these formulations produced the hoped-for advantages of cell-mediated medication delivery: Superior tissue distribution and longer persistence of ATV and RTV than are obtained with conventional formulations.
The nano-ART advantage was demonstrated with both single- and multiple-dose administration. Compared with animals that received conventional formulations of the same drugs, mice that received nano-formulations exhibited antiretroviral concentrations that were 7 (ATV) to 13 (RTV) times higher in blood serum and 9 (ATV) to 41 (RTV) times higher in the liver, 2 weeks after the last dose. The medications were also found in the lung and spleen at this point in animals that received nano-ART, while they had dropped to undetectable levels in animals that received the conventional formulations.
Similarly, the nano-ART advantage was sustained over the course of 8 weeks with weekly dosing. Serum and tissue concentrations of ATV and RTV stabilized after the second week and remained stable until 2 weeks after the final injection. The concentrations produced by nano-ART surpassed those produced by conventional formulations by multiples of 3 (ATV) to 14 (RTV) in the lung; 13 (ATV) to 271 (RTV) in the liver (see Figure); and intermediate amounts in the serum, kidney, and spleen. To confirm that nano-ART was working as intended in the living animals, the researchers documented by fluorescence labeling that the medications localized within macrophages (called Kupffer cells) in the liver.
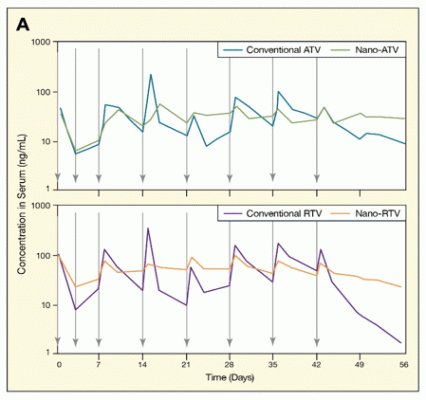
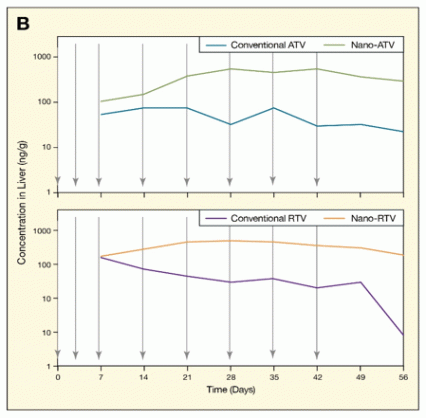
Figure. Nano-formulations of Atazanavir (ATV) and Ritonavir (RTV) Enhance Medication Delivery Weekly injections (vertical arrows) of 50 milligram per kilogram of nano-formulated ATV or RTV into mice resulted in medication concentrations in the blood serum (Panel A) and liver (Panel B) that were higher overall and more stable than those yielded by the medications in their conventional formulations.
- Text Description of Graphic
-
The figure shows 4 line graphs indicating the concentration of 2 different formulations (conventional drug or nano-formulation) of the antiretroviral drugs atazanavir (ATV) and ritonavir (RTV) in blood serum (panel A) and liver tissue (panel B) of mice. The vertical (y)-axes show the concentrations of the drugs in serum (as nanogram per milliliter) or tissue (as nanogram per gram). The horizontal (x)-axes show the time (in days) at which the drugs were injected into the mice and their concentrations measured. Vertical arrows at 3, 7, 14, 21, 28, 35, and 42 days indicate when 50 milligram per kilogram of the drugs were injected into the mice. The graphs in Panel A show that concentrations of both drugs in blood fluctuated over time, spiking after each drug injection. However, this effect was less pronounced in mice injected with the nano-formulations of ATV (green line, top graph) or RTV (orange line, bottom graph), and drug concentrations stayed higher even 2 weeks after the last injection than in mice injected with the conventional formulations of ATV (blue line, top graph) and RTV (purple line, bottom graph). The graphs in Panel B show that drug levels in liver tissues were consistently and about 2- to 10-fold higher after injection with the nano-formulations of ATV (green line, top graph) and RTV (orange line, bottom graph) than after injection with the conventional formulations of the two drugs (blue and purple lines in top and bottom graphs, respectively).
To extend these findings to animals more similar to humans, the researchers injected the nano-ART formulations into two rhesus macaques. Following three intramuscular doses given over 7 days, one animal sustained plasma concentrations of ATV and RTV that are associated with therapeutic efficacy in human patients for at least 14 days, and plasma levels remained detectable for at least 5 weeks.
Dr. Alnouti says that these findings in mice and monkeys mark an important milestone in the progress of nano-ART toward potential clinical use. On the basis of the results, he hypothesizes that weekly or monthly administration of fully developed nano-ART might treat HIV disease more conveniently and more effectively than current regimens.
The Nebraska research team is now seeking ways to optimize the advantages of nano-ART. Their current goal is to create nano-ART formulations that can attack HIV in the brain and lymphatic system. The formulations of ATV and RTV tested in the recent study did not improve transfer of the drugs across the blood–brain barrier into the central nervous system; and the lymphatic system is another region where HIV eludes conventional ART and accumulates in viral reservoirs.
Strategies the researchers are exploring to meet these challenges include adding folic acid or a small piece of viral protein to their current nano-ART formulation in hopes to stimulate macrophages to take up more of the drugs and transport them in larger quantities into hard-to-reach tissues.
Dr. Rao Rapaka, chief of NIDA’s Chemistry and Physiological Systems Research Branch says that Dr. Alnouti’s results to date are promising, yet cautions that they represent very early steps toward clinical use of nano-ART. “These preliminary findings are encouraging, but there’s more work to be done. The team will now have to gather enough evidence to demonstrate the drug concentrations in target organs as well as the effectiveness and the stability of the nano-ART drug formulation,” Dr. Rapaka notes.
For his part, Dr. Alnouti expresses confidence in the approach. “I think nano-ART is the future of HIV treatment,” he says. “And if we can deliver ART drugs into the brain and lymph nodes, this will mean a paradigm shift in HIV treatment. We might even be able to eradicate the virus.”
This study was supported by NIH grants DA028555 and DA026146.
Source:
Gautam, N.; Roy, U.; Balkundi, S. et al. Preclinical pharmacokinetics and tissue distribution of long-acting nanoformulated antiretroviral therapy. Antimicrobial Agents and Chemotherapy 57(7):3110-3120, 2013. Full text
