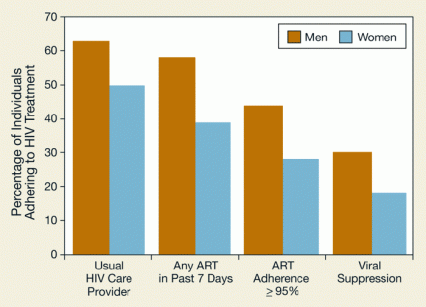
 Figure. Women Ex-Detainees With HIV Are Less Engaged in HIV Care Than Their Male Counterparts Six months after being released from jail, women were less likely than men to have a regular HIV care provider, to take antiretroviral therapy (ART) medication, to adhere to ART, or to have viral suppression (undetectable levels of the virus in their blood).
Figure. Women Ex-Detainees With HIV Are Less Engaged in HIV Care Than Their Male Counterparts Six months after being released from jail, women were less likely than men to have a regular HIV care provider, to take antiretroviral therapy (ART) medication, to adhere to ART, or to have viral suppression (undetectable levels of the virus in their blood).Women who are infected with HIV and are transitioning back to communities after serving jail time are less likely than their male counterparts to have a regular HIV care provider, to take and regularly adhere to an HIV medication regimen, and to have suppression of the virus, a NIDA-sponsored study reports. The findings add to previous evidence that HIV treatment for women leaving jail should be tailored to their specific needs.
- Text Description of Graphic
-
The figure shows a bar graph indicating the proportion of former jail detainees infected by HIV who adhered to treatment for the virus. The vertical (y)-axis shows the percentage of detainees adhering to HIV treatment, and the horizontal (x)-axis shows the type or measure of adherence, that is, having an HIV care provider, any ART in the past 7 days, an ART adherence of 95 percent or more, and suppression of the virus. The orange bars represent the percentages of men and the light blue bars percentages of women adhering to HIV treatment. As shown by the differences in bar heights between the two groups, consistently fewer women than men leaving jail adhered to HIV treatment. Fewer women saw their usual HIV care provider (a difference of 13 percentage points relative to the percentage for men), had any ART in the past 7 days (difference of 19 percentage points), showed ART adherence of equal or more than 95 percent (difference of 16 percentage points), and showed viral suppression (difference of 12 percentage points).
Dr. Jaimie Meyer with the AIDS Program at Yale University School of Medicine, in New Haven, Connecticut, and colleagues compared HIV treatment outcomes of 590 men and 277 women 6 months after their release from jail. The men and women were participants in a demonstration project to design and test innovative ways to link HIV-infected detainees to community-based care after their release from jail. The project, Enhancing Linkages to HIV Primary Care and Services in Jail Settings, was conducted at 10 sites in 9 states.
The researchers found that, 6 months post-release, only half of the women reported having a regular HIV care provider, compared with almost two-thirds of the men (see Figure). Only 39 percent of the women reported taking any antiretroviral medication in the past 7 days versus 58 percent of the men, resulting in less than 1 in 5 of the women having suppression of the virus compared with almost 1 in 3 of the men. Compared with their pre-incarceration status, women were less likely (18 percent versus 26 percent), and men were more likely (30 percent versus 25 percent), to have viral suppression 6 months after leaving jail. Viral suppression means that treatment has reduced blood levels of the virus to an undetectable level, although it does not indicate that the patient’s HIV is cured. The women’s findings were striking because all the study participants received intensive case management services specifically designed to link them to HIV care in communities.
The researchers note that women who are arrested and incarcerated often have more severe medical, psychiatric, and substance use disorders than their male counterparts. Many are in relationships that expose them to risk for violence and limit their autonomy in making health care decisions.
For instance, according to the study, on entering jail, about two-thirds of the women reported using cocaine in the past 30 days, while less than one-half of the men did. The researchers also say that not living in stable housing and substance use are both often coupled with psychiatric disorders, and these adverse situations disproportionately affect women.
These and other challenges likely affected women’s ability to seek and keep involved in treatment, the researchers say. Hence, HIV intervention packages that respond to the women’s particular problems and needs as they transition from jail back to independent life may yield better outcomes. For example, engagement in mental health and addiction treatment services and use of appropriate psychiatric medications both increase involvement in antiretroviral therapies.
As Dr. Meyer explains, “Interventions designed specifically for women living with HIV achieve optimal outcomes when they simultaneously and comprehensively address the issues that distract women from engaging in care.”
This study was supported by NIH grants DA017072 and DA033858.
Source:
Meyer, J.P.; Zelenev, A.; Wickersham, J.A. et al. Gender disparities in HIV treatment outcomes following release from jail: results from a multicenter study. American Journal of Public Health 104(3):434-441, 2014. Full text
