A can-do attitude, ability to cope with potential triggers for drug use, readiness to change, and participation in self-help programs are major assets for people trying to recover from cocaine addiction. In a NIDA-funded study, each of these factors markedly increased patients' odds for attaining or maintaining abstinence, or both, during 2 years of intensive outpatient treatment and continuing care. On the liability side of the ledger, symptoms of depression were associated with continued drug use and with relapse (see Figure).
The study, conducted by Dr. James McKay and colleagues at the University of Pennsylvania and the Philadelphia Veterans Affairs Medical Center, yields insights that clinicians can use to evaluate patients with cocaine addiction and plan their treatment and aftercare. Among their detailed findings, the researchers discovered that the list of factors that help patients become abstinent overlaps, but is not identical with, the list of factors that support extending established abstinence.
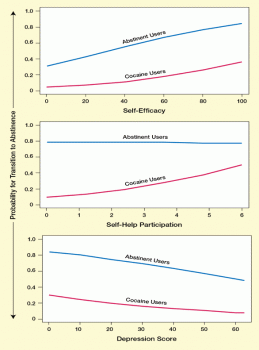 Figure. Self-Efficacy, Self-Help Participation, and Depression Affect the Likelihood of Future Abstinence Among study participants who enrolled in intensive outpatient programs for treatment of cocaine addiction, high self-efficacy raised the likelihood of becoming and staying abstinent. Increased self-help participation raised the likelihood of future abstinence among those currently using cocaine but did not promote continued abstinence among those who had already stopped using the drug. More severe depression decreased the odds of future abstinence in both current and former users of cocaine.
Figure. Self-Efficacy, Self-Help Participation, and Depression Affect the Likelihood of Future Abstinence Among study participants who enrolled in intensive outpatient programs for treatment of cocaine addiction, high self-efficacy raised the likelihood of becoming and staying abstinent. Increased self-help participation raised the likelihood of future abstinence among those currently using cocaine but did not promote continued abstinence among those who had already stopped using the drug. More severe depression decreased the odds of future abstinence in both current and former users of cocaine.
- Text Description of Graphic
-
The figure shows three line graphs indicating the likelihood of staying or becoming abstinent for former and current users of cocaine, respectively, who were enrolled in intensive outpatient treatments for cocaine addiction, depending on how the users scored on self-efficacy, self-help participation, and depression. The vertical (y)-axis shows the probability of transitioning to (or staying in) abstinence (as relative values ranging from 0 to 1). The horizontal (x)-axes show the self-efficacy score, ranging from 0 to 100 (top graph); the self-help participation score, ranging from 0 to 6 (middle graph); and the depression score, ranging from 0 to 65 (bottom graph). As shown in the top graph, the likelihood of abstinent former users of cocaine to stay abstinent (indicated by a blue line) steadily rose from about 0.35 at a self-efficacy score of 0 to about 0.8 at a self-efficacy score of 100; current cocaine users’ likelihood of becoming abstinent (shown by a red line), although generally lower, also rose from less than 0.1 at a self-efficacy score of 0 to about 0.25 at a self-efficacy score of 100. As shown in the middle graph, abstinent former cocaine users’ likelihood of staying abstinent (shown by a blue line) remained unchanged at about 0.8 across all seven scores for self-help participation, whereas current cocaine users’ likelihood of becoming abstinent (indicated by a red line), although generally lower, gradually rose from about 0.1 with a self-help participation score of 0 to about 0.55 with a self-help participation score of 6. As shown in the bottom graph, abstinent former cocaine users’ likelihood of staying abstinent (shown by a blue line) declined from about 0.85 at a depression score of 0 to about 0.5 at a depression score of 65; current cocaine users’ likelihood of becoming abstinent (shown by a red line) also declined from 0.3 at a depression score of 0 to less than 0.1 at a depression score of 65.
Allies for Abstinence
Dr. McKay's team interviewed 776 patients addicted to cocaine at intervals of 3 or 6 months, starting when the patients had completed 2 to 4 weeks of intensive outpatient therapy, and ending 24 months later. At each interview, the researchers recorded the patients' recovery status (cocaine use or abstinence) and assessed 14 factors that substance abuse treatment interventions commonly target. The researchers analyzed these data to determine which factors influenced whether the patient would still be in the same recovery status at their next interview or would have transitioned from one status to the other.
Most patients persisted in the same recovery status throughout the study, but 20 percent transitioned from use to abstinence, and 20 percent transitioned in the other direction at some point. Five of the assessed factors greatly influenced patients' prospects for recovery.
Self-efficacy (confidence in one's ability to overcome recovery challenges) helped patients to both achieve and maintain abstinence. Among patients who were currently using cocaine at one interview, those with high self-efficacy had a 35 percent likelihood of being abstinent at the next interview, while those with low self-efficacy had essentially no chance. Among patients who were abstinent at one interview, those with high self-efficacy had more than 80 percent likelihood of still being abstinent at the next interview, while those who reported low self-efficacy had less than 40 percent likelihood of abstinence.
"People with high self-efficacy are confident in their ability to successfully employ the coping skills they've been taught in treatment, and, consequently, they do not resort to substance abuse, for example, whenever they are stressed or experience negative emotions," Dr. McKay explains.
Frequent participation in self-help programs and endorsement of self-help principles strongly benefited only those participants who were currently using cocaine. Patients' odds of transitioning from current use to abstinence at the next follow-up were 50 percent among those who reported regularly attending self-help meetings and keeping in contact with other self-help participants, and less than 20 percent among those reporting little or no self-help participation. Patients who were already abstinent had an 80 percent chance of extending their abstinence regardless of their participation in self-help programs.
"These results indicate that it is particularly important for relapsed patients to continue or resume participation in self-help programs. The results suggest it is not as crucial for abstinent individuals to continue with self-help attendance. The results shouldn't be construed to indicate that abstinent individuals do not need to attend self-help anymore. We looked only at outcomes at the next follow-up. It is quite possible that drop-offs in self-help participation in abstinent people could eventually lead to relapse at later time points," Dr. McKay notes.
Similar to self-help participation, coping ability in situations associated with elevated risk for relapse and readiness to change both were associated with improved odds of becoming abstinent, but not of extending abstinence. Among patients who were using cocaine, high versus low coping skills increased the likelihood of transitioning to abstinence by the next follow-up interview by 50 percentage points. Current users of cocaine who reported high readiness to change had a 40 percent likelihood of being abstinent at the next follow-up interview, while those who reported low readiness to change had little or no likelihood of being cocaine free at the follow-up.
Depressive illness increased the difficulty of both achieving and maintaining abstinence. Current users of cocaine who reported high levels of symptoms on the Beck Depression Inventory (BDI) assessment had a 10 percent chance of being abstinent 3 or 6 months later, compared with 30 percent among those with low BDI scores. Among currently abstinent patients, those with low depression scores had an 80 percent chance of remaining abstinent at the next interview, whereas those with high depression scores had less than a 60 percent chance of remaining cocaine free.
"This finding is of potential clinical utility," notes Dr. McKay. "If you're treating cocaine dependence, it's worth monitoring depression, because a high level of depression puts people at increased risk for relapse." Individuals with these elevated risks could then receive special treatments tailored to their needs to prevent a relapse, Dr. McKay says. Moreover, he notes that the study's findings may also be relevant for patients in other treatment settings, such as during post-treatment follow-up periods after inpatient or residential programs, or during and after standard outpatient care.
Commitment and Support
In addition to self-efficacy, self-help participation, readiness to change, and depression, other treatment-malleable factors predicted a patient's recovery trajectory to a lesser degree. These included:
- Commitment to abstinence: Patients committed to total abstinence versus those with less stringent abstinence goals were 12 percentage points more likely both to be newly abstinent and to still be abstinent at the next follow-up interview.
- Family and social support: Higher levels of general social support from family and friends improved patients' odds both for becoming abstinent and for maintaining abstinence by 10 to 15 percentage points.
One surprising finding of the study was that family and social problems and medical and legal problems—which are included in the widely used Addiction Severity Index (ASI)—affected cocaine abstinence less than self-efficacy and self-help participation did.
"The ASI domains are important factors, but they're not the strongest predictors of substance use," says Dr. McKay.
Consistent with earlier reports, the researchers found that older age and lower cocaine and alcohol use at the start of treatment were associated with abstinence from cocaine use. Dr. McKay and colleagues also found that men were more likely than women to transition from cocaine use to abstinence. Although other studies have reported that a person's history of treatment for drug use also affects patients' odds for achieving and maintaining abstinence, it had no such effect in the present study.
"These data really begin to tell a story about what might be important factors or targets in substance abuse treatments," says Dr. Will M. Aklin, the study's program officer in NIDA's Division of Clinical Neuroscience and Behavioral Research. Now that these factors have been identified, "treatment should be focused on those factors that correlate with recovery from cocaine abuse," Dr. Aklin notes.
This study was supported by NIH grants DA029062 and DA020623.
Reference
McKay, J.R.; Van Horn, D.; Rennert, L. et al. Factors in sustained recovery from cocaine dependence. Journal of Substance Abuse Treatment 45(2):163-172, 2013. Full text
